Liver & Bile Duct Surgery
What is the liver?
The liver is the largest solid organ in the body. It has several functions (“What does the liver do?” ). The liver receives its blood from the heart and filters blood coming from the intestines. The outflow of the liver returns blood to the heart and lungs and excretes bile to the bowel.
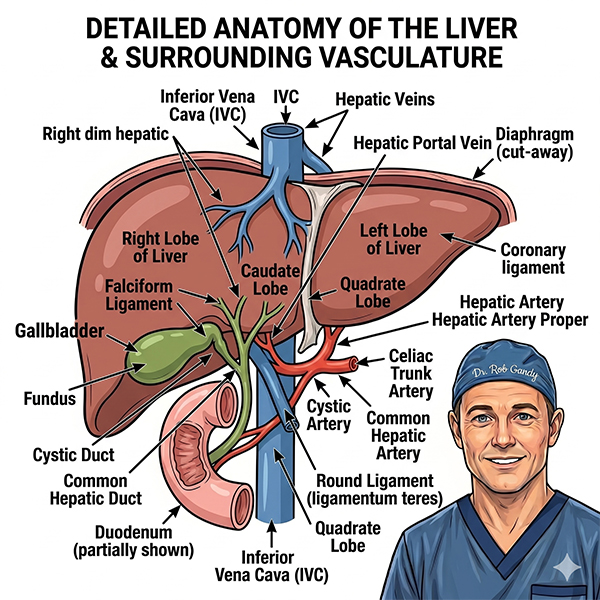
What are the bile ducts?
The bile ducts are a tree of channels throughout the liver. The small branches are inside the liver and these channels pass bile to the main trunk located outside the liver. The main trunk (common bile duct), joins with the gallbladder duct and then enters the first part of the small intestine.
What does bile do?
Bile is like a detergent that turns greasy fat into a fatty emulsion, which can then be absorbed by the bowels.
What does the liver do?
The liver performs a variety of metabolic functions including:
- Removing waste products, hormones, drugs, and toxins
- Producing bile to aid digestion (transported to the bowel in the bile ducts)
- Processing nutrients absorbed from the bowel
- Storing nutrients
- Stabilising blood sugar
- Making proteins and blood clotting factors
- Removing bacteria and red blood cells from the circulation
Why might I need bile duct or liver surgery?
Non-cancerous conditions
- Bacterial infections can cause a liver abscess in the liver which may need draining.
- Simple cysts may cause pressure on the liver or stomach and need draining
- Non-cancerous growths in the liver (haemangioma, adenoma, focal nodular hyperplasia) may need observation and rarely removal
- Stones may form in the liver or bile ducts that may need removal of the bile ducts or associated liver.
- Non-cancerous narrowing of the bile ducts may need removal or biliary reconstruction.
- Injury to the bile ducts at gallbladder surgery may need to be repaired or reconstructed.
Cancerous conditions (tumours)
- Cancers of the bile ducts may need removal, often with part of the liver, pancreas or sometimes both.
- Cancers from other sites that have spread to the liver (liver metastases)
- Cancers that have formed in the liver (primary liver cancer)
Who can have liver or bile duct surgery?
Up to around 70% of the liver can be removed, in healthy people. The liver can regenerate, but if too much liver is removed, or if the damage to the liver has already occurred, the liver can fail. Older people can undergo liver surgery provided they have a good level of fitness.
How is traditional liver surgery performed?
All liver surgery is major surgery and is associated with many risks. It is possible for keyhole surgery to be performed on the liver for some non-cancerous conditions and a small percentage of people with liver cancers. The ultimate goal of liver surgery is safety and for this reason most liver operations are formed in a traditional open approach.
After a J-shaped incision is made over the liver. The area of the liver to be removed is then marked using an ultrasound probe. It may be necessary to block the blood flow to the part of the liver to be removed. The liver is then carefully divided with cautery, titanium clips and silk ligatures.
What happens if the bile duct needs to be removed?
If the bile duct is to be removed, the remainder of the duct is reconnected directly to the bowel. This is done by suturing the bowel wall to the bile duct. In most cases this part of the bowel is diverted from the flow of food by forming a junction in the bowel (Roux-en-Y)
What are the risks of liver surgery?
Around 10% of patients may develop a complication after liver surgery. The risks are greater as the amount of liver removed increases.
During surgery, the main risk is bleeding and the need for a blood transfusion.
After surgery, the complications include
- Bleeding (most commonly seen in major liver resection)
- Wound infection
- Bile leakage (from the liver or bile duct joins)
- Fluid accumulation in the abdomen (until the liver function returns)
- Pneumonia or kidney failure
- blood clots in the legs or lung (injections are given to thin the blood slightly to prevent this)
- Liver failure (if too much liver is removed or the remaining liver is of poor quality)
How long will I need to be in hospital and what is the recovery like?
Recovery in hospital usually takes 5-10 days with the first 1-2 days I the intensive care ward. Most people can eat and drink within the first two days, but some of the pain medications may cause nausea and constipation. The amount of post-operative pain experienced may be variable and combination of tablets, wound catheters and patient controlled injections into the drip.
How soon can I go back to normal activity?
Depending on your level of fitness you may need help at home after leaving hospital. You will be assessed by physio and occupational therapist prior to discharge. If extra services are required, a hospital social worker may be able to assist. Most people can return to work in 3-4 weeks. Light exercise may be resumed after 2 weeks and strenuous activity after 6weeks.
What if the liver tumours cannot be removed?
There are multiple options liver tumours that cannot be removed. While the results of these treatments are not as long lasting as removing the tumour, they may benefit some people
- Chemotherapy - the use of drugs to halt growth or shrink a tumour
- Radiotherapy - the use of x-rays to kill or halt growth of a tumour.
- Ablation - using microwaves, radiofrequency waves or electricity (Nanoknife) to try destroy a tumour.
- Embolization - blocking the blood supply to a tumour, often combined with chemotherapy.
- Liver transplantation - In Australia, strict criteria govern the use of liver transplantation as a treatment for liver cancer. Liver transplantation is limited to patients with primary liver cancer, if transplantation is an option you will be referred to the Australian national liver transplantation Unit at Royal Prince Alfred Hospital.
