Hernia Surgery
Hernia Surgery in Sydney: Types, Symptoms, and Modern Treatments
Can a hernia heal on its own?
No. A hernia is a physical defect in the abdominal wall. It will not resolve without surgical intervention and typically enlarges over time. If left untreated, it can lead to life-threatening complications like bowel obstruction or strangulation.
What is a Hernia?
A hernia occurs when an internal organ or fatty tissue pushes through a weakened spot in the surrounding muscle or connective tissue (the abdominal wall). This creates a balloon-like sac that may contain a loop of intestine.
Common Types of Hernia
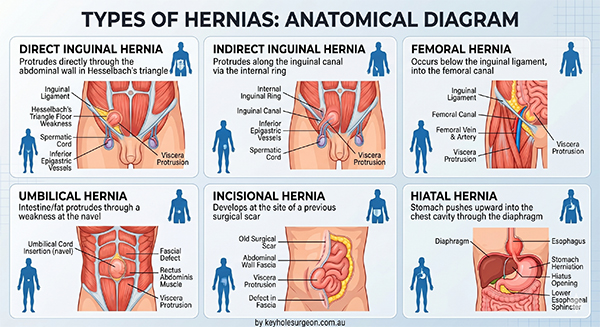
The most common types of hernia are
- Inguinal (inner groin)
- Ventral or Incisional (resulting from an incision)
- Femoral (outer groin)
- Umbilical (belly button),
- Hiatal (upper stomach)
Symptoms: How to Tell if You Have a Hernia
The most common sign is a visible bulge that may disappear when you lie down or reappear when you cough, strain, or lift heavy objects.
- Pain/Discomfort:Often felt at the site of the protrusion, especially when lifting.
- The "Vanishing" Lump:A lump in the groin that is felt while standing but disappears at rest.
- Red Flag Symptoms:Excruciating pain, nausea, vomiting, or a lump that becomes firm/red. These indicate strangulation or obstruction and require immediate emergency care.
Hernia vs. Muscle Strain
It can be difficult to distinguish between a sports-related muscle strain and a true hernia. While a strain is a tear in the muscle fibers, a hernia is a hole in the abdominal wall.
Expert Note: Dr. Gandy uses medical history, physical exams, and occasionally MRI or ultrasound to differentiate between the two. Learn more about Hernia vs. Strain here.
Surgical Treatment Options
Surgery is the only definitive cure for a hernia. Dr. Gandy specializes in two primary approaches:
- Laparoscopic Hernia Surgery (Keyhole)
This is the modern standard for most patients. Using small incisions and a video camera, Dr. Gandy repairs the abdominal wall from the inside.
- Benefits:Less post-operative pain, smaller scars, and a significantly faster return to daily activities.
- Materials:Usually involves a combination of sutures and polypropylene mesh to reinforce the repair.
- Open Hernia Surgery
A traditional approach involving a larger incision directly over the hernia.
- Best For:Very large hernias or when the hernia has returned after prior surgery, the incision can be easily hidden, or for patients specifically requesting a meshless repair.
Recovery and Returning to Normal Life
Most hernia repairs are performed as day-stay procedures, meaning you can go home the same day you have surgery.
- First 24 Hours:You can eat immediately and are encouraged to walk around and shower.
- Work & Sport:
- Office Work:Usually 1 week.
- Low-Impact Sport:1 week.
- Heavy Lifting/Contact Sports:4–6 weeks.
- Detailed Timeline:See our Week-by-Week Recovery Chart.
Frequently Asked Questions
Can I have a hernia repair without mesh?
Yes. While "meshless" repairs have a higher rate of recurrence (the hernia coming back), Dr. Gandy is happy to discuss non-mesh options for patients who have specific concerns.
What are the risks of surgery?
While rare (less than 2%), risks include infection, bleeding, or injury to the bladder or nerves. Recurrence occurs in approximately 1% of cases.
Why Choose Dr. Robert Gandy for Hernia Surgery in Sydney?
When selecting a surgeon for hernia repair, experience and surgical volume are the two most critical factors in reducing the risk of recurrence. Dr. Robert Gandy is recognized as one of the highest-volume hernia surgeons in Australia, offering a rare combination of technical precision and patient-focused care.
Key Credentials & Expertise:
- 20 Years of Surgical Experience:With two decades in the field and over 10 years as a specialist consultant in Sydney, Dr. Gandy brings a wealth of clinical judgment to complex cases.
- High-Volume Specialist:High-volume surgeons typically achieve better patient outcomes and lower complication rates. Dr. Gandy performs hundreds of hernia repairs annually.
- Minimally Invasive Focus:He specializes in advanced laparoscopic (keyhole) techniques, which prioritize faster recovery, reduced post-operative pain, and long-term abdominal wall integrity.
- Personalized Surgical Pathways:Whether you require a standard mesh repair or are seeking a meshless (suture-only) hernia repair, Dr. Gandy tailors the procedure to your specific health profile and lifestyle goals.
Practice Locations
Dr. Gandy provides specialized surgical care across major Sydney hubs, ensuring accessibility for patients in Randwick, the Sydney CBD, and surrounding regions.
How much does hernia surgery cost?
The exact cost of your hernia repair depends on your health insurance and the hospital you choose.
- Initial Consultation Fees
Before any surgery, an initial consultation is required to assess your hernia and discuss the best surgical approach (including laparoscopic or meshless options).
- New Patient Consultation:$250 (An out-of-pocket cost of $174 after the Medicare rebate).
- Post-Operative Care:Most post-operative consultations are free and included in your surgical care plan.
- Bulk-Billed Clinic:A bulk-billed option is available at the surgical outpatients clinic at Prince of Wales Public Hospital. (Please note: Waiting times can be up to three months, and you may be seen by a supervised surgical trainee).
- Surgical Fees by Insurance Status
We prioritize transparent pricing so you can make an informed decision regarding your healthcare without hidden surprises.
Option A: Private Health Insurance ("No Gap" Surgery)
If you have private hospital cover, Dr. Gandy participates in several “Gap cover” schemes. Under a No Gap arrangement, you will have zero out-of-pocket costs for the surgical and anaesthetic fees.
- Medibank Private & HCF Members:Special "No Gap" arrangements are available for hernia repairs performed at East Sydney Private Hospital. Depending on your level of cover (Gold/Silver), your hospital excess may also be waived, resulting in a completely free admission. For more information click the links below
No Gap Endoscopy Program Surgeon
No Gap General Surgery Program Surgeon
- Other Health Funds:Fees are determined by the Australian Medical association (AMA) schedule.
- Note:Depending on your specific policy, you may still need to pay your standard hospital excess on the day of admission.
Option B: Public Hospital (Medicare)
For patients with a valid Australian Medicare card, hernia surgery at the Prince of Wales Public Hospital is performed free of charge.
- Gandy supervises these surgeries and some post-operative care is provided by his specialized surgical training team.
- Patient may use their private insurance in the public hospital to have surgery personally performed by Dr Gandy and his fees are charged directly to the health fund under the “No Gap” arrangement
- Access to the public hospital list is prioritized by clinical urgency, and wait times will apply, regardless of insurance status.
Option C: Self-Funded (Uninsured) Patients
If you do not have private health insurance but wish to avoid public hospital waiting lists, you can choose to be treated as a private patient at Prince of Wales Private Hospital or East Sydney Private Hospital.
- What you pay:You will be responsible for the hospital facility fee and theatre costs (which varies by hospital), a surgical fee, and anaesthetic fee on admission.
- Rebates:A proportion of the surgical and anaesthetic fees will attract a rebate from Medicare.
- Next Steps:We assist all self-funded patients in obtaining a comprehensive estimate of all costs before proceeding. Quotes cannot be confirmed prior to consultation, until the specific item number is confirmed.
Our Commitment to Transparency
In alignment with the Medical Cost Finder initiatives, our practice is committed to upfront, clear communication regarding the value and cost of your surgical care. Following your consultation, you will receive a detailed, written quotation outlining all expected fees, Medicare rebates, and any out-of-pocket expenses.
