Obesity & Weight Loss Treatment: A Comprehensive Guide
Obesity is a medical diagnosis defined as a Body Mass Index (BMI) greater than 30. However, this number is a rough measure; excess weight and body fat put people at risk for various chronic health conditions and a lower life expectancy.
Obesity in New South Wales
In Australia, two-thirds (67%) of adults are overweight. The rate of clinical obesity has risen dramatically in New South Wales, from 1 in 5 people in 1995 to over 1 in 3 people in 2017-2018. This increase is linked to changes in our society, including a rise in sedentary jobs and the marketing of unhealthy foods.
Understanding Weight Gain
Weight gain and obesity result from a sustained energy imbalance, where the energy intake from food and drinks is greater than the energy expended through physical activity. This imbalance is influenced by genetics, biology, and lifestyle.
Energy is expended in three main ways:
- Basal metabolic activity: The energy your body uses to function at rest (e.g., heart beating, brain working). This is often referred to as your metabolism.
- Thermic effect of food: The energy used to break down and absorb food. Processed foods require less energy to digest.
- Physical activity: The energy used for movement, including both daily tasks and exercise.
Health and Social Impacts of Obesity
Obesity is a major risk factor for several health problems, including cardiovascular disease, type 2 diabetes, certain musculoskeletal conditions, and some cancers. As excess weight increases, so does the risk of developing these conditions.
The text also highlights the significant social and emotional impacts of obesity. Many people experience distress, anxiety, and low self-esteem related to their weight. This can lead to:
- Anxiety about shopping for clothes or using public transport.
- Feeling self-conscious in social situations, like eating in a cafe or going to the gym.
- Social stigmatization and reduced career progression.
Why Is Weight Loss So Difficult?
Losing a significant amount of weight and keeping it off is very challenging. Our bodies are biologically programmed to store energy efficiently, and dieting can trigger a "famine mode," which makes the body even better at storing fat and causes strong hunger cravings. Additionally, exercise can be difficult due to joint pain or the social stigma associated with being overweight.
How Is Obesity Measured?
Obesity is commonly measured using the Body Mass Index (BMI), which is an internationally recognized standard. However, BMI is a limited tool. It does not account for factors like gender, muscle mass, or body fat distribution, and it may not fully assess a person's risk of obesity-related diseases.
Body mass index (BMI)
The following standard cut-off points are used for adults (age 20 and over):
|
BMI |
|
|
20-25 |
Normal |
|
25-30 |
Overweight |
|
30-35 |
Obese |
|
35-40 |
Severely Obese |
|
40-50 |
Morbidly Obese |
|
50+ |
Super Obese |
Waist Circumference & Bariatric Surgery Candidacy
While not a direct indicator for weight loss surgery, waist circumference is an alternative way to assess the risk of developing obesity-related chronic diseases. A higher waist measurement is associated with an increased risk of chronic disease.
|
Increased risk |
substantially increased risk |
|
|
Men |
94cm |
102cm |
|
Women |
80cm |
88cm |
Am I a Candidate for Weight Loss Surgery?
You may be a candidate for weight loss surgery if you meet the following criteria:
- You have a BMI over 35.
- You have a BMI over 30 and are experiencing negative health effects from your weight.
- You are more than 45 kg above your ideal body weight.
- You have been unable to achieve a healthy, sustained weight through supervised diet and exercise.
- You are highly motivated and committed to long-term lifestyle changes.
The team at the BodyFree clinic considers not only your BMI but also your overall health and any existing medical diagnoses.
Surgical Options for Weight Loss
There are several surgical procedures designed to help with weight loss, each with different benefits and considerations.
- Endoscopic Bariatric Procedures: These include the gastric balloon and endoscopic stomach suturing. They are generally less durable and result in less weight loss than traditional surgical options.
- Laparoscopic Adjustable Gastric Band: This procedure, once very common, is now rarely performed due to the high rate of patient side effects.
- Laparoscopic Sleeve Gastrectomy: A safe and durable procedure where a portion of the stomach is removed, making it smaller. This is a permanent procedure that also reduces hunger cravings. Patients typically lose 60-70% of their excess weight by two years.
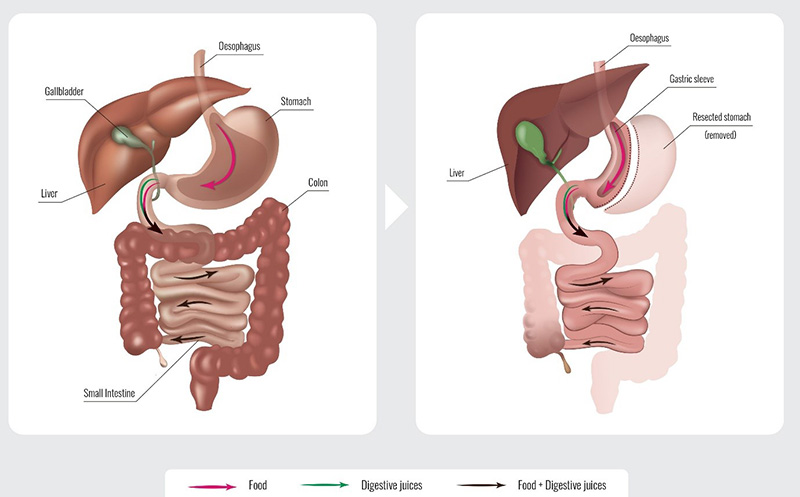
- Laparoscopic Gastric Bypass: This procedure reduces stomach size and reroutes the small intestine to limit both food intake and absorption. It is associated with the highest weight loss and rates of diabetes remission but requires a strong commitment to long-term follow-up and nutritional supplements.
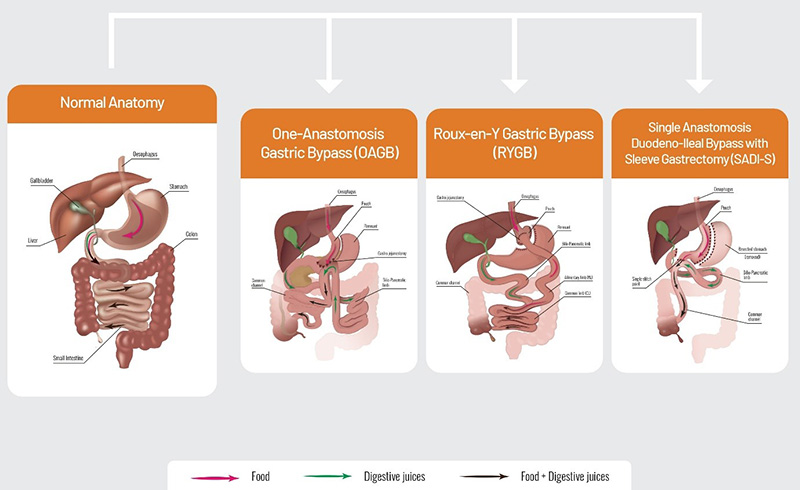
- Revision Bariatric Surgery: This is an option for patients who have had a previous weight loss procedure, most often a gastric band, and are experiencing complications, weight regain, or insufficient weight loss.
The Surgical Process & Recovery
Bariatric surgery is a specialized procedure performed in a hospital setting. It is almost always completed using keyhole (laparoscopic) surgery, which allows for faster recovery.
Hospital Stay:
- Sleeve Gastrectomy: 1-2 nights.
- Gastric Bypass: 1-2 nights
Post-Surgery Diet: A specialized 6-week diet is crucial for healing and initial weight loss. Adherence to this diet is one of the most important aspects of a successful outcome. The diet progresses in stages:
- First two weeks: Protein-rich fluids
- Weeks 2-4: Pureed foods
- Weeks 4-6: Soft/mushy diet
You must avoid high-calorie foods, high-sugar foods, processed foods, alcohol, and soft drinks. It is also critical to stay hydrated by drinking at least 1.5 litres of fluid per day.

Cost of Weight Loss Surgery
At BodyFree Weight Loss Clinic, we offer all-inclusive pricing for a fixed fee, so you won't have to worry about unexpected costs. The pricing is divided into two clear options based on your insurance status.
For Patients with Private Health Insurance
If your private health insurance covers Bariatric Surgery (Gastric Sleeve or Gastric Bypass) and you have not had a previous bariatric procedure, our all-inclusive program starts at $3,990.
This package includes:
- Surgical and physician consultations.
- The surgery itself (Gastric Sleeve, Gastric Bypass).
- Surgical assistant and anaesthetist fees.
- A hospital stay of 2-3 nights.
- Five dietitian consultations.
- 24 months of ongoing surgical follow-ups at our clinic.
Please Note: You may have to pay an additional excess to your health fund. Revision surgery has a higher fee due to its complexity. To check your coverage, provide your insurer with these item numbers:
- 31575 for Gastric Sleeve
- 31572 for Gastric Bypass
For Patients Without Private Health Insurance (Medicare Only)
Bariatric surgery is still an option even without private health insurance. We offer two programs:
- All-Inclusive Program: For $14,990, this program provides the same comprehensive care as our insured patients receive.
- Basic Program: Starting at $13,990, this option includes:
- Initial surgical and dietitian consultations.
- Gastric Sleeve surgery, including surgical assistant and anaesthetist fees.
- A 2-night hospital stay.
- One post-operative dietitian and one post-operative surgical consultation.
Important: Telehealth consultations may incur additional fees.
For more information or to book an appointment, please contact us at 1300 507 989 or use the online contact form.
Revision weight loss surgery has a higher set fee due to its complexity, please contact us for a quote.
Seeking More Information
The best sources of information are people with personal experience with weight loss surgery or your general practitioner. Your GP can provide a referral for a discussion with the team at the BodyFree Weight Loss Clinic.
