Pancreatic Cyst
Understanding Pancreatic Cysts: A Guide for Patients
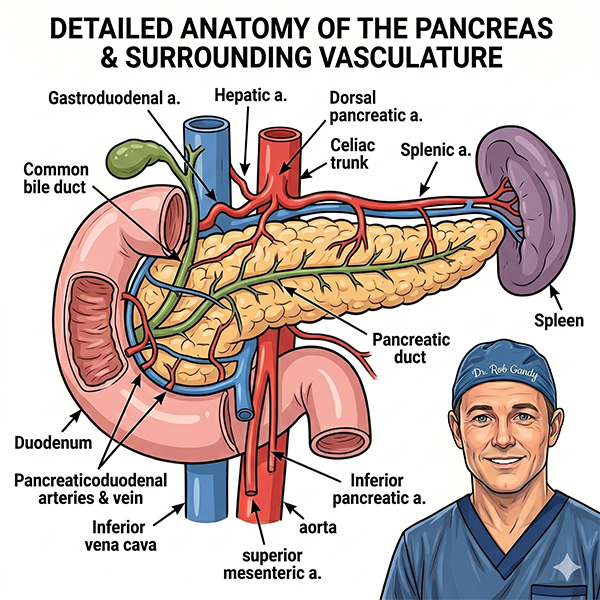
Finding out you have a pancreatic cyst can be unsettling, but it is important to know that most pancreatic cysts are not cancerous and many do not require surgery. Often discovered "incidentally" during a CT or MRI scan for an unrelated issue, these cysts require expert assessment to determine the best path forward.
What Exactly is a Pancreatic Cyst?
A cyst is a sac-like pocket of fluid. In the pancreas, they fall into two main categories:
- True Cysts: These have a cellular lining and may have the potential to grow.
- Pseudocysts: These lack a lining and usually form as a result of inflammation (pancreatitis) or injury.
Common Types & Risk Levels
Not all cysts are created equal. Specialists categorize them based on their "malignant potential" (the risk of becoming cancerous).
| Cyst Type | Typical Patient | Risk Level | Action Plan |
|---|---|---|---|
| Serous (SCN) | Often women | Very Low | Observation only; surgery rare. |
| Mucinous (MCN) | Women over 40 | Moderate | Often removed due to future risk. |
| IPMN | Men & Women | Variable | Close monitoring or surgery if "worrisome." |
| Pseudocyst | Post-Pancreatitis | Non-Cancerous | Drainage only if causing pain or infection. |
Do I Have Symptoms?
Most pancreatic cysts are "silent" and cause no symptoms. However, if a cyst grows large or blocks a duct, you may experience:
- Abdominal pain radiating to the back.
- Nausea or vomiting.
- Unexplained weight loss.
- Jaundice (yellowing of the skin/eyes)—this is rare and requires immediate review.
Diagnosis & Next Steps
If a cyst is detected, your specialist will likely use the following "toolkit" to get a clearer picture:
- Specialist Imaging: An MRI/MRCP provides high-detail images of the pancreatic ducts to see if the cyst is connected to them.
- Endoscopic Ultrasound (EUS): A thin tube with an ultrasound probe is passed into the stomach. This allows the doctor to take a tiny fluid sample (Fine Needle Aspiration) for lab analysis.
- Multidisciplinary Team (MDT) Review: Your results are reviewed by a panel of surgeons, radiologists, and gastroenterologists to ensure the most accurate recommendation.
The Goal of Surveillance: For many patients, "watchful waiting" with a scan every 6–12 months is the safest and most effective way to manage a low-risk cyst.
When is Treatment Necessary?
Treatment (usually surgery) is typically only recommended if:
- The cyst is causing significant symptoms (pain or duct blockage).
- Testing shows pre-cancerous cells or "high-risk" features.
- The cyst is growing rapidly.
Specialist Assessment with Dr. Gandy
If you have been diagnosed with a pancreatic cyst, an expert evaluation is essential for peace of mind and clear direction.
Ready to discuss your results?
Dr. Gandy provides comprehensive assessment and advanced surgical treatment for all pancreatic conditions.
- Phone: 02-8599-4360
- Location: Prince of Wales Private Hospital, Randwick, NSW
Frequently Asked Questions
Does a pancreatic cyst mean I have cancer?
No. Most pancreatic cysts are benign. While some have the potential to become cancerous over many years, the majority are harmless "incidental findings." The purpose of your specialist appointment is to identify which category your cyst falls into.
If it isn’t cancer, why do I need regular scans?
Think of it like monitoring a mole on your skin. We perform "surveillance" (periodic MRI or CT scans) to ensure the cyst isn’t changing in size or developing internal features that might suggest a shift in risk level.
What is the difference between a simple cyst and a pseudocyst?
A "true" cyst is a collection of fluid that grew on its own. A pseudocyst is usually a side effect of inflammation (pancreatitis); it is essentially a pocket of "leaked" digestive juices that the body has walled off.
What does "Watchful Waiting" involve?
If your cyst is small and shows no "worrisome features," we typically recommend a scan every 6 to 12 months. If the cyst remains stable for several years, the frequency of these scans may decrease.
Can I prevent pancreatic cysts through diet?
While diet doesn't directly cause or cure cysts, maintaining a low-fat diet and limiting alcohol can reduce the workload on your pancreas and prevent inflammation, which is particularly important if you have a pseudocyst.
Is the surgery for a pancreatic cyst major?
Pancreatic surgery is significant, which is why we only recommend it when the risk of the cyst turning into cancer outweighs the risk of the procedure. Many procedures can now be performed using keyhole (laparoscopic) techniques, which lead to faster recovery times.
How to Prepare for Your Appointment
To get the most out of your consultation with Dr. Gandy, please bring:
- Copies of your imaging: Both the written reports and the actual images (on a disc or digital link) from your CT or MRI.
- Medical History: A list of any previous abdominal issues or family history of pancreatic conditions.
Glossary: Understanding Your Pathology & Imaging Reports
When you receive a scan report, you may see complex terminology. Here is a breakdown of what those terms actually mean in plain English:
- Aspiration (FNA): The process of using a very fine needle to withdraw a small amount of fluid from the cyst for testing.
- Ductal Communication: This describes whether the cyst is "plugged into" the main tubes of the pancreas. IPMNs typically communicate with the ducts, while MCNs usually do not.
- Endoscopic Ultrasound (EUS): A procedure where a specialist uses a scope to look at the pancreas from inside the stomach. It provides much higher detail than a standard CT scan.
- Incisional/Keyhole Surgery: Also known as laparoscopic surgery. This uses small cuts and a camera rather than one large incision, typically resulting in a faster recovery.
- Malignant Potential: The statistical likelihood that a specific type of cyst could turn into cancer over time.
- MDT (Multidisciplinary Team): A group of different specialists (surgeons, radiologists, oncologists) who meet to discuss your specific case to ensure the best treatment plan.
- Septations: Thin "walls" or divisions inside the cyst. A "unilocular" cyst has one chamber; a "multilocular" cyst has several.
- Worrisome Features: A specific medical term used by radiologists to describe things like a thickened cyst wall or a cyst larger than 3cm. These features don't always mean cancer, but they do mean the cyst needs closer attention.
What to do if you see these terms on your report
If your report contains words like "septated," "mucin-producing," or "dilated duct," don't panic. These are descriptive markers that help Dr. Gandy categorize the cyst. They are pieces of a puzzle, not a final diagnosis on their own.
Booking Your Consultation
Dr. Gandy specializes in interpreting these complex reports and providing clear, actionable advice. If you have your results ready, we can move quickly to the next stage of assessment.
- Call to Book: 02-8599-4360
- Online Referral: https://www.keyholesurgeon.com.au/online-sydney-randwick.html
